What is hydrocephalus in infants?
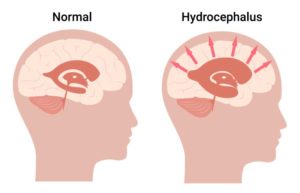
Hydrocephalus occurs when cerebrospinal fluid (CSF) builds up in cavities called ventricles inside the brain. This extra fluid widens the ventricles and puts pressure on the brain’s tissues.
 In Greek, “hydro” means head, and “cephalus” means water. In many cases, hydrocephalus is a birth injury, but sometimes it is caused by a congenital defect (birth defect).
In Greek, “hydro” means head, and “cephalus” means water. In many cases, hydrocephalus is a birth injury, but sometimes it is caused by a congenital defect (birth defect).
Think of CSF as liquid bubble wrap. It protects and cushions the brain and spine. Typically, the body produces the same amount of CSF that it absorbs.
However, when the flow or absorption of CSF is blocked, the fluid can build up and cause pressure in the brain.
The pressure can stop the brain from working the way it should. It can also cause brain damage or, in the worst-case scenario, death. When left untreated, hydrocephalus is fatal in 50% of patients.
The good news is that treatment, including surgery, can return CSF to normal levels and help children with pediatric hydrocephalus live full lives.
Hydrocephalus is the single most common reason for brain surgery in young children.
Types of pediatric hydrocephalus
There are two main types of hydrocephalus in infants:
- Communicating hydrocephalus happens when the flow of CSF is blocked at the brain’s surface after leaving the ventricles. The term “communicating” means that the CSF can still flow between the ventricles (cavities).
- Non-communicating hydrocephalus occurs when the flow of CSF gets blocked along one or more of the skinny passages that connect the ventricles. This condition is also called obstructive hydrocephalus.
Hydrocephalus is sometimes classified as acquired or congenital. Congenital means present at birth.
Genetic factors and events that happen when a baby is growing inside the womb can cause congenital hydrocephalus. In rare cases, symptoms first appear in adulthood.
Congenital hydrocephalus occurs in 2 of every 1,000 births in the United States, according to UCLA Health.
Acquired hydrocephalus develops after birth. It can be caused by a head injury or brain tumor.
What causes hydrocephalus in infants?
Pediatric hydrocephalus is often a symptom of another health problem. Sometimes the condition develops during pregnancy, and in other cases, it develops after birth.
The most common causes of each type of hydrocephalus are outlined below.
- Aqueductal stenosis (narrowing of a channel in the brain known as the aqueduct of Sylvius or the cerebral aqueduct)
- Brain malformations
- Spina bifida (a condition in which a baby's spine does not form properly before birth)
- Brain tumors
- Head injuries (including those from medical negligence)
- Infections such as meningitis
- Intraventricular hemorrhage (brain bleed)
Aqueductal stenosis is the most common cause of congenital hydrocephalus.
The cerebral aqueduct connects the third and fourth ventricles. When this narrows, as in aqueductal stenosis, it interferes with the flow of cerebrospinal fluid and leads to a buildup of fluid in the ventricles. This is how aqueductal stenosis causes hydrocephalus.
Premature infants are at risk of brain bleeds and, as a result, hydrocephalus. A pediatric neurologist or neurosurgeon may be able to pinpoint the cause of hydrocephalus in a baby.
In many cases, pediatric hydrocephalus is preventable and can be considered a birth injury. If you believe your child’s hydrocephalus could have been prevented, contact one of our team members for a free case review.
What are the symptoms of hydrocephalus in infants?
Babies with hydrocephalus often have unusually large heads. This is because the head often grows in size to handle the buildup of cerebrospinal fluid. It leads to increased cranial pressure.
Here are some symptoms of hydrocephalus in infants.
- A rapid increase in head size
- Bulging soft spot (fontanel)
- Prominent scalp veins
- Thin and glistening scalp
- Eyes stuck looking down (“setting sun”)
- Irritability
- Seizures
- Sleepiness
- Vomiting
An older child with hydrocephalus may experience different symptoms because of the increased pressure in their head.
Signs of hydrocephalus in toddlers and older children can include:
- A change in personality
- Delays in walking or talking
- Headaches
- Memory problems
- Nausea
- Poor coordination
- Vision problems
- Vomiting
Children with this condition may also start having problems in school. They often struggle to get up in the morning and stay awake.
In some cases, symptoms are obvious. In others, the signs are less noticeable and progress slowly.
Parents who think their child may have hydrocephalus should seek immediate medical attention.
Sadly, when left untreated, hydrocephalus can be fatal. However, with early diagnosis and prompt medical care, children have a good chance of recovering.
Diagnosing pediatric hydrocephalus
When a medical professional suspects hydrocephalus in a newborn, they will perform a physical exam and review the child’s medical history.
A pediatrician might measure the baby’s head. This measurement is known as the head circumference. They will track the increase in head circumference and note any sudden changes
In an older child, the physician might ask about any developmental delays.
Doctors often use these brain imaging tests to confirm pediatric hydrocephalus:
- Computed tomography (CT scan) uses X-rays and computer technology to image the brain.
- Magnetic resonance imaging (MRI) uses magnets, radio waves, and a computer to show images of the brain.
They may order more scans so they can see if the condition is getting worse.
Using ultrasounds to diagnose hydrocephalus in babies in the womb
An MRI or prenatal ultrasound can sometimes spot hydrocephalus in a baby growing inside the womb. An ultrasound uses sound waves to make an image of the inside of a person's body.
An ultrasound can show the size of the ventricles inside a baby’s brain.
Congenital hydrocephalus usually develops in the third trimester of pregnancy. As a result, ultrasounds performed earlier may not detect the condition.
Treatment options for infants with hydrocephalus
Medical treatment for a hydrocephalus baby will depend on several factors, including the child’s age, symptoms, and overall health.
The goal of hydrocephalus treatment is to lessen the pressure inside the baby’s head.
Doctors from different specialties typically decide the course of treatment for hydrocephalus in infants. For example, pediatric neurosurgeons, neurologists, radiologists, and ophthalmologists may help develop a treatment plan.
The majority of infants with hydrocephalus will need surgery. Some of them will also be given a type of medication known as a diuretic that helps eliminate extra water from the body.
Children with this condition may need medical monitoring for the rest of their lives.
The most common surgical treatments for pediatric hydrocephalus are:
Shunts
A pediatric neurosurgeon implants a shunt in the child’s brain. This flexible tube transports extra cerebrospinal fluid from the brain to another part of the body, like the belly, where it can be absorbed.
A shunt is the most common treatment for hydrocephalus. However, children with shunts often get infections and need repeat surgeries if the shunt becomes blocked or stops working.
According to the National Institute of Neurological Disorders and Stroke, 40% of shunts in children malfunction in the first year after placement and 10% per year after that.
Children with shunts generally have 2-5 operations to maintain the devices during their lifetimes. While some children only need one surgery, others may require multiple shunt revisions in a single year.
Endoscopic third ventriculostomy (ETV)
A neurosurgeon makes a small hole in the skull and guides an endoscope (a long, thin tube with a camera) through the brain. The surgeon makes a hole in the affected ventricle, which allows the CSF to bypass the blockage.
Surgeons usually perform ETV in children older than 2 with non-communicating hydrocephalus.
Choroid plexus cauterization (CPC)
A neurosurgeon burns (cauterizes) brain tissue that produces CSF to lower the amount of fluid flowing into the ventricles. The procedure is mainly used in children younger than 2.
The thought of your child undergoing brain surgery can be scary. However, keep in mind that many children’s hospitals have been treating hydrocephalus in infants for decades. Plus, today’s pediatric surgeons use minimally invasive techniques that lower the risk of complications.
Many parents are also comforted by the fact that children are under anesthesia for these procedures. After surgery, children may feel weak and tired or sore at the site of the shunt. They typically stay in the hospital for a few days as they recover. In most cases, school-age children can return to school in several weeks.
Prognosis for babies with hydrocephalus
When a baby is diagnosed with hydrocephalus, parents often worry about their child's health and what the future may hold. The essential thing to remember is that every child is unique and will face different obstacles.
Babies with shunts may need multiple shunt revisions as they adjust to treatment. These brain surgeries can impact a child’s development.
Some babies with hydrocephalus are diagnosed with other co-occurring conditions, including cerebral palsy, spina bifida, seizures, and vision problems. As a result, these children may take longer to hit developmental milestones and often have sensory issues and other challenges.
However, with medical treatment, different types of therapy, and special education services, most children with hydrocephalus live full, vibrant lives. Many are still able to socialize with friends, play sports, graduate high school, and attend college.
Infants who have surgery for hydrocephalus and live to age 1 will not have a shortened life expectancy because of the condition, according to UCLA Health.
Raising a child with hydrocephalus
Once parents get over the shock of a hydrocephalus diagnosis, they may feel sad, angry, or helpless. These are all normal emotions.
Parents can ease feelings of helplessness by working with their child's health care team to develop a treatment plan. Additionally, they can take steps to prevent shunt infections at home and take their child to regular medical appointments.
Parents of a baby with hydrocephalus should also learn what to do in an emergency.
Parents and other caregivers should call the child’s doctor if they notice these symptoms:
- Change in behavior
- Continuing headaches
- Fever
- Increased sleepiness
- Persistent vomiting
- Redness along the track of the shunt
They should call 9-1-1 if the child has these symptoms:
- Inability to wake
- Seizures
- Sundowning of eyes (downward gaze)
Support groups for pediatric hydrocephalus
Parents raising children with hydrocephalus often benefit from talking to caregivers dealing with similar issues. Hydrocephalus Association has a helpline that parents can call for support and information about available resources. The group also has trained volunteers who give peer support and a community network that provides opportunities for families to connect.
Many other support groups and organizations provide resources and a sense of community to families raising children with disabilities.
One important thing to remember is that you are not alone.
In addition, children with hydrocephalus often benefit from special education and various therapies, including physical therapy and occupational therapy.
Financial support may be available through government assistance, foundations, or legal compensation.
Get pediatric hydrocephalus legal help
Medical mistakes can cause harm to an otherwise healthy baby before, during, or shortly after childbirth. When these errors cause head trauma, they can lead to hydrocephalus and be considered medical negligence.
For example, when a baby is stuck in the birth canal, doctors may use forceps or vacuum extraction to help deliver the child. Babies born by vacuum delivery are at risk of hydrocephalus, as are children with forceps delivery complications.


In addition, a doctor who fails to diagnose or treat certain prenatal infections puts a child at risk of developing hydrocephalus.
While hydrocephalus is treatable when diagnosed early, it usually affects children for the rest of their lives and can cause permanent impairments and health complications.
A family that believes their child’s hydrocephalus was caused by a preventable mistake during childbirth might qualify for a birth injury lawsuit.
A birth injury lawsuit allows caregivers to seek compensation for:
- Assistive devices
- Medications
- Physical therapy
- Speech therapy
- Surgery
- Other expenses
Get a free case review to find out whether you can take legal action for your child’s hydrocephalus.




